- Doctors & Departments
-
Conditions & Advice
- Overview
- Conditions and Symptoms
- Symptom Checker
- Parent Resources
- The Connection Journey
- Calm A Crying Baby
- Sports Articles
- Dosage Tables
- Baby Guide
-
Your Visit
- Overview
- Prepare for Your Visit
- Your Overnight Stay
- Send a Cheer Card
- Family and Patient Resources
- Patient Cost Estimate
- Insurance and Financial Resources
- Online Bill Pay
- Medical Records
- Policies and Procedures
- We Ask Because We Care
Click to find the locations nearest youFind locations by region
See all locations -
Community
- Overview
- Addressing the Youth Mental Health Crisis
- Calendar of Events
- Child Health Advocacy
- Community Health
- Community Partners
- Corporate Relations
- Global Health
- Patient Advocacy
- Patient Stories
- Pediatric Affiliations
- Support Children’s Colorado
- Specialty Outreach Clinics
Your Support Matters
Upcoming Events
Mental Health Town Hall
Tuesday, April 23, 2024Join Children’s Hospital Colorado pediatric experts for a virtual...
-
Research & Innovation
- Overview
- Clinical Trials
- Q: Pediatric Health Advances
- Discoveries and Milestones
- Training and Internships
- Academic Affiliation
- Investigator Resources
- Funding Opportunities
- Center For Innovation
- Support Our Research
- Research Areas

It starts with a Q:
For the latest cutting-edge research, innovative collaborations and remarkable discoveries in child health, read stories from across all our areas of study in Q: Advances and Answers in Pediatric Health.


Arm Injury
Get Care Now
From emergency to urgent care to 24/7 pediatric advice, we’re here to help in the heat of moment.
- Injuries to the arm (shoulder to hand)
- Injuries to a bone, muscle, joint or ligament
- Excluded: muscle pain caused by too much exercise or work (overuse). Covered in Arm Pain.
- Excluded: finger injury only. See that care guide.
Types of Arm Injuries
- Fractures are broken bones. A broken collarbone is the most common broken bone in children. It's easy to notice because the collar bone is tender to touch. Also, the child cannot raise the arm upward.
- Dislocations happen when a bone is pulled out of a joint. A dislocated elbow is the most common type of this injury in kids. It's caused by an adult quickly lifting a child by the wrist or hand. It can also be caused by suddenly pulling a child toward you. Mainly seen in 1 to 4 year olds. It's also easy to spot. The child will hold his arm as if it were in a sling. He will keep the elbow bent and the palm of the hand down.
- Sprains are stretches and tears of ligaments.
- Strains are stretches and tears of muscles (such as a pulled muscle).
- Muscle Overuse. Muscle pain can occur without an injury. There is no fall or direct blow. Muscle overuse is from hard work or sports (such as a sore shoulder).
- Muscle bruise from a direct blow
- Bone bruise from a direct blow
- Skin Injury. Examples are a cut, scratch, scrape or bruise. All are common with arm injuries.
Pain Scale
- Mild: your child feels pain and tells you about it. But, the pain does not keep your child from any normal activities. School, play and sleep are not changed.
- Moderate: the pain keeps your child from doing some normal activities. It may wake him or her up from sleep.
- Severe: the pain is very bad. It keeps your child from doing all normal activities.
Call 911 Now
- Serious injury with many broken bones
- Major bleeding that can't be stopped
- Bone is sticking through the skin
- You think your child has a life-threatening emergency
Go to ER Now
- Can't move the shoulder, elbow or wrist at all
- Looks like a broken bone (crooked or deformed)
- Looks like a dislocated joint
- Large deep cut that will need many stitches
Call Doctor or Seek Care Now
- Can't move the shoulder, elbow or wrist normally
- Collarbone is painful and can't raise arm over head
- Can't open and close the hand normally
- Skin is split open or gaping and may need stitches
- Cut over knuckle of hand
- Age less than 1 year old
- Cut or scrape and no past tetanus shots. Note: tetanus is the "T" in DTaP, TdaP, or Td vaccines.
- Severe pain and not better 2 hours after taking pain medicine
- You think your child has a serious injury
- You think your child needs to be seen, and the problem is urgent
Contact Doctor Within 24 Hours
- Very large bruise or swelling
- Pain not better after 3 days
- Dirty cut or hard to clean and no tetanus shot in more than 5 years
- Clean cut and no tetanus shot in more than 10 years
- You think your child needs to be seen, but the problem is not urgent
Contact Doctor During Office Hours
- Injury limits sports or school work
- Pain lasts more than 2 weeks
- You have other questions or concerns
Self Care at Home
- Bruised muscle or bone from direct blow
- Pain in muscle from minor pulled muscle
- Pain around joint from minor stretched ligament
- Minor cut or scrape
Care Advice for Minor Arm Injuries
What You Should Know About Minor Arm Injuries:
- During sports, muscles and bones get bruised.
- Muscles get stretched.
- Here is some care advice that should help.
Pain Medicine:
- To help with the pain, give an acetaminophen product (such as Tylenol).
- Another choice is an ibuprofen product (such as Advil). Ibuprofen works well for this type of pain.
- Use as needed.
Small Cut or Scrape Treatment:
- Use direct pressure to stop any bleeding. Do this for 10 minutes or until bleeding stops.
- Wash the wound with soap and water for 5 minutes. Try to rinse the cut under running water.
- Gently scrub out any dirt with a washcloth.
- Use an antibiotic ointment (such as Polysporin). No prescription is needed. Then, cover it with a bandage. Change daily.
Cold Pack for Pain:
- For pain or swelling, use a cold pack. You can also use ice wrapped in a wet cloth.
- Put it on the sore muscles for 20 minutes.
- Repeat 4 times on the first day, then as needed.
- Reason: helps the pain and helps stop any bleeding.
- Caution: avoid frostbite.
Use Heat After 48 Hours:
- If pain lasts over 2 days, put heat on the sore muscle.
- Use a heat pack, heating pad or warm wet washcloth.
- Do this for 10 minutes, then as needed.
- Reason: increase blood flow and improve healing.
- Caution: avoid burns.
Rest the Arm:
- Rest the injured arm as much as possible for 48 hours.
What to Expect:
- Pain and swelling most often peak on day 2 or 3.
- Swelling should be gone by 7 days.
- Pain may take 2 weeks to fully go away.
Call Your Doctor If:
- Pain becomes severe
- Pain is not better after 3 days
- Pain lasts more than 2 weeks
- You think your child needs to be seen
- Your child becomes worse
Care Advice for Minor Arm Injuries

To put on a sling you first need to have a triangle-shaped bandage. Many first aid kits have a triangle bandage.
- Find the two ends of the triangle that are farthest apart. These are the ends that you will tie around the neck.
- Lay the arm down the middle of the triangle.
- Take the two ends of the triangle that are farthest apart and tie them behind the neck (a square knot is best, but any knot will do).
- Make sure the wrist is at a level higher than the heart.
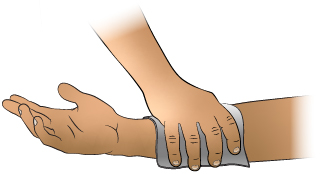
- Apply direct pressure to the entire wound with a sterile gauze dressing or a clean cloth. Once the bleeding has stopped, cover with an adhesive bandage or gauze.
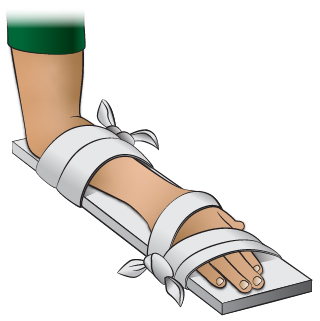
- Keep the hand and wrist from moving by placing them on a rigid splint (see drawing).
- Tie several cloth strips around hand/wrist to keep the splint in place. You can use a roll of gauze or tape instead of cloth strips.
Notes:
- You can make a splint from: a wooden board, magazine folded in half, folded-up newspaper, cardboard, or a pillow.
- If you have no splinting materials, then support the injured arm by resting it on a pillow or folded up blanket.
- After putting on the splint, apply a cold pack or an ice pack (wrapped in a towel) to the area.
Copyright 2000-2024. Schmitt Pediatric Guidelines LLC.
Disclaimer: this health information is for educational purposes only. You, the reader, assume full responsibility for how you choose to use it.

Get to know our pediatric experts.

Shane Wo, MD
Emergency Medicine - Pediatric, Pediatrics
Patient ratings and reviews are not available Why?

Travis Murray, MD
Orthopaedic Surgery

Jessica Parker, DO
Emergency Medicine - Pediatric, Pediatrics
Patient ratings and reviews are not available Why?

James Brown, MD
Emergency Medicine - Pediatric, Pediatrics
Patient ratings and reviews are not available Why?



 720-777-0123
720-777-0123





