- Doctors & Departments
-
Conditions & Advice
- Overview
- Conditions and Symptoms
- Symptom Checker
- Parent Resources
- The Connection Journey
- Calm A Crying Baby
- Sports Articles
- Dosage Tables
- Baby Guide
-
Your Visit
- Overview
- Prepare for Your Visit
- Your Overnight Stay
- Send a Cheer Card
- Family and Patient Resources
- Patient Cost Estimate
- Insurance and Financial Resources
- Online Bill Pay
- Medical Records
- Policies and Procedures
- We Ask Because We Care
Click to find the locations nearest youFind locations by region
See all locations -
Community
- Overview
- Addressing the Youth Mental Health Crisis
- Calendar of Events
- Child Health Advocacy
- Community Health
- Community Partners
- Corporate Relations
- Global Health
- Patient Advocacy
- Patient Stories
- Pediatric Affiliations
- Support Children’s Colorado
- Specialty Outreach Clinics
Your Support Matters
Upcoming Events
Colorado Hospitals Substance Exposed Newborn Quality Improvement Collaborative CHoSEN Conference (Hybrid)
Monday, April 29, 2024The CHoSEN Collaborative is an effort to increase consistency in...
-
Research & Innovation
- Overview
- Pediatric Clinical Trials
- Q: Pediatric Health Advances
- Discoveries and Milestones
- Training and Internships
- Academic Affiliation
- Investigator Resources
- Funding Opportunities
- Center For Innovation
- Support Our Research
- Research Areas

It starts with a Q:
For the latest cutting-edge research, innovative collaborations and remarkable discoveries in child health, read stories from across all our areas of study in Q: Advances and Answers in Pediatric Health.


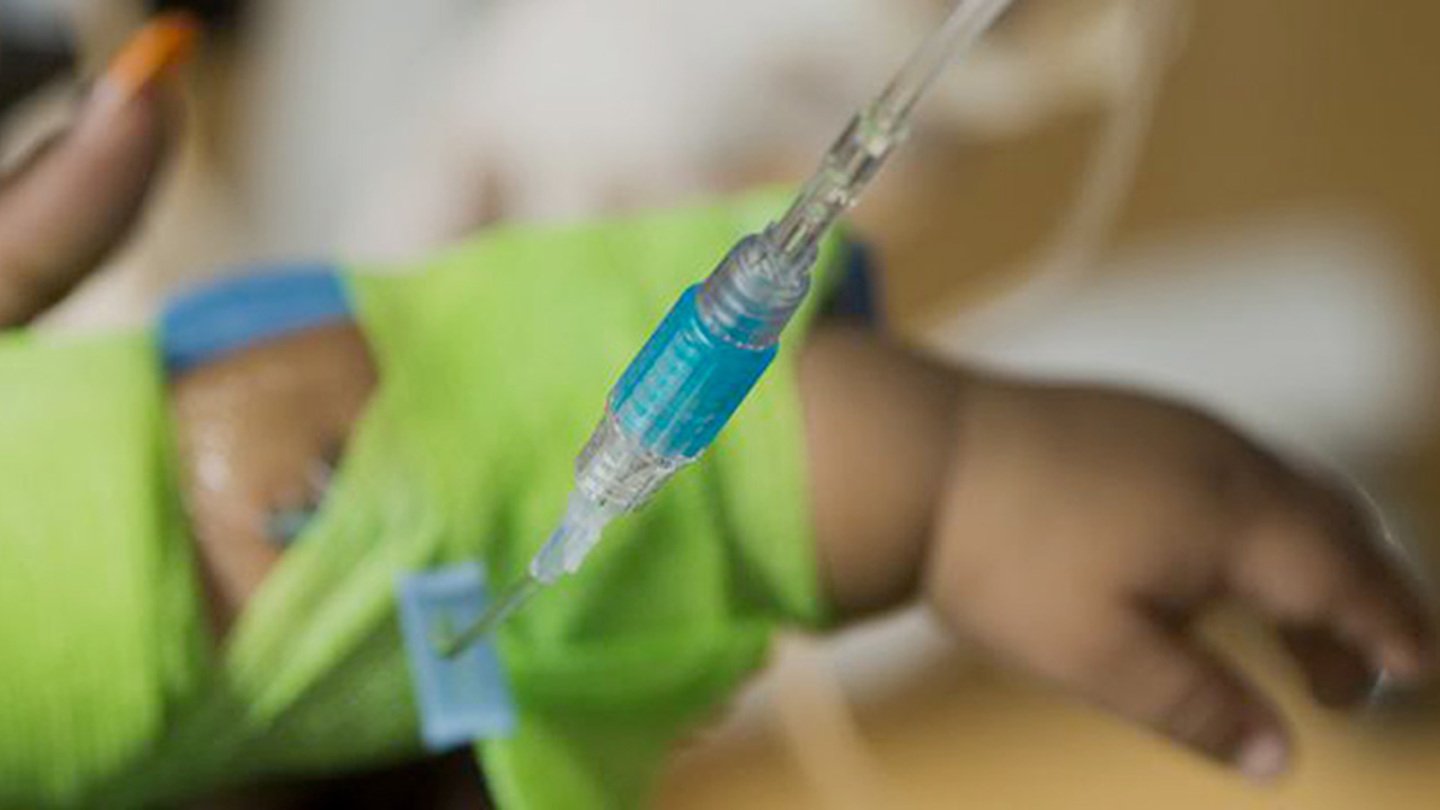

About the Pediatric Blood and Marrow Transplant and Cellular Therapy Program
When your child needs a blood or bone marrow transplant or cellular therapy treatment, you want to find the best care possible. That’s why our Pediatric Blood and Marrow Transplant and Cellular Therapy Program team is committed to the highest standards of quality, the latest and most proven treatments, and the overall care and well-being of your child and family.
Our team is the region's most experienced pediatric blood and marrow transplant and cellular therapy (BMT) program. We have performed more than 1,100 bone marrow transplants and have a growing cellular therapy program offering new, effective and less toxic therapies for a variety of diseases. Our providers specialize in pediatric blood and marrow transplants and cellular therapy, so you can trust that your child is in good hands.
Learn more about the bone marrow transplant processWhy choose us for blood and marrow transplant or cellular therapy care
Excellent blood and marrow transplant outcomes and expertise
The International Bone Marrow Transplant Registry, the National Marrow Donor Program (NMDP) and U.S. News & World Report recognize Children's Colorado as meeting the highest standards of 100-day and one-year post-BMT survival compared to other U.S. pediatric BMT programs. See our BMT survival rates.
Our BMT Program has been continuously accredited by the Foundation for Accreditation of Cellular Therapy (FACT) since 2001. This certification is granted to a limited number of hospitals and is based on patient outcomes, patient volumes, qualified staff, appropriate facilities and having a comprehensive quality assurance program that meets current national FACT standards. The standards indicate that our transplant team has been consistently recognized through national peer review for high-quality patient care and laboratory performance for bone marrow transplant.
Our program is also an approved transplant site of the NMDP, the Children's Oncology Group (COG) and the Pediatric Transplantation and Cellular Therapy Consortium.
1,100+
Bone marrow transplants performed
10
Years of our program meeting or exceeding international standards (out of 10 years evaluated)
28+
Years of pediatric bone marrow transplant experience
Cutting-edge cellular therapy
Our pediatric specialists offer a range of cellular therapy options, including chimeric antigen receptor (CAR) T cells and virus-directed T cells. T cells are a type of white blood cell that develop from stem cells in the bone marrow. They help fight infection and can fight cancer.
CAR-T cells: For this type of cellular therapy, we draw blood from a patient to collect circulating T cells, which are an important part of the body’s immune system. Next, using a non-contagious virus, we genetically engineer these T cells to make specialized proteins on the T cell surface. These engineered T cells, called CAR-T cells, are capable of recognizing certain cancer cells. The CAR-T cells are then infused back into the patient and attach to specific proteins on the surface of cancer cells. The CAR then triggers the T cells to kill the cancer cell. Our team has extensive experience with both commercially available and locally manufactured CAR-T cells, and we can safely manufacture new types of CAR-T cells that are not available elsewhere.
Virus-directed T cells: After a bone marrow transplant, it takes a while for the new immune system to recognize cells that are infected with certain viruses. Often, viruses from the Herpesvirus family, which are known to cause diseases such as mononucleosis (“mono”), upper respiratory tract infections, cold sores and roseola, never fully go away after the first infection. Rather, the immune system keeps them at bay.
When the immune system is recovering after a bone marrow transplant, these viruses can cause significant infections, which sometimes lead to very severe complications for a bone marrow transplant patient. Similar to the development of CAR-T cells, we can use engineered T cells from the blood of the stem cell donor or another individual to produce cells that recognize the virus-infected cells and kills them. This therapy can be lifesaving for people with these types of infections.
Who we treat at the Pediatric Blood and Marrow Transplant and Cellular Therapy Program
We treat patients from birth to 26 years old who could benefit from a blood and marrow transplant or cellular therapy.
Specialized BMT care for teenagers and young adults
Research has shown that teens and young adults with cancer do better when treated on pediatric protocols and in a pediatric setting. Stem cell sources and therapy regimens often differ between adult and pediatric institutions and may affect outcomes. Additionally, pediatric oncologists and bone marrow transplant specialists are more experienced with managing any potential long-term complications after therapy.
What does our Pediatric Blood and Marrow Transplant and Cellular Therapy Program offer?
Our multidisciplinary BMT program includes:
- Consultation, evaluation, treatment and follow-up care
- BMT-trained pediatric physicians, nurse practitioners and physician assistants
- Board-certified pediatricians and pediatric hematologists/oncologists
- Pediatric radiation oncologists
- Dedicated, BMT-trained nursing staff
- Dedicated pediatric BMT-trained pharmacists
- A HEPA-filtered, positive pressure 24-bed inpatient BMT unit with the capacity to expand to 48 beds when needed
- Transplant coordinators who guide patients and advocate for them through the entire transplant experience – coordinating care from entry into the Program through transition back to the primary care provider
- BMT-specific outpatient team and clinic services
- Fertility preservation services
- Palliative care services focused on symptom management, quality of life and how you or your child is best treated
- Technology and on-site facilities to procure and process stem cells from marrow, peripheral blood and cord blood
- Availability of both autologous (a patient's own stem cells) and allogeneic (another person as the donor stem cells) transplant methods and expertise
- Numerous state-of-the-art local, national and international clinical trials in pediatric hematopoietic stem cell transplant and investigational drug availability
- Care within the context of a large, highly specialized pediatric academic medical center with all sub-specialties on site and available throughout the transplant care
- A Children's Oncology Group (COG) Transplant Center
- A National Marrow Donor Program (NMDP) Transplant Center
- A member of the Pediatric Transplantation and Cellular Therapy Consortium
- Access to all unrelated donor registries (NMDP, Caitlin Raymond International, Cord Blood) for stem cell products
Support services for your family
Our program offers a full range of support services for patients and families, including:
- Patient and family support from social workers, clinical psychologists, physical and recreational therapists, teachers, child life specialists, art therapists, pastoral care and others
- BMT patient and family resources to help you better understand what to expect
- A financial coordinator to assist physicians and families with financial approval
- Established contracts for transplant care with numerous insurers
- Access to private apartments at Brent's Place, a safe, clean housing facility specifically designed for immune-compromised patients that is located near the hospital
- A Spanish-speaking care team and additional foreign language translators to facilitate communication and understanding of treatment plans for all patients
- Comprehensive late-effects and survivorship services designed to help young patients lead healthier lives post-transplant and transition to adult care when the time comes
Pediatric bone marrow transplantation and cellular therapy research and innovation
Members of our team are actively involved in pediatric bone marrow transplant and cellular therapy research with the goal of improving outcomes in children. Our team performed its first cord blood transplant in 1996, early in the investigation of this now common stem cell source. Today, our ongoing research projects focus on optimizing the success of BMT for many pediatric disorders in cancer, immunodeficiencies, sickle cell disease and rare metabolic conditions.
Read about our most recent cancer and blood disorder research.
For healthcare professionals
Our team members are committed to providing excellent service to patients and providers through an efficient call-back and evaluation for urgent referrals. Streamlined communication occurs before, during and after transplantation. Our expert team is regularly consulted by providers around the country and the world for the specialized care that we can deliver here. Get more information for healthcare professionals or apply to our hematology oncology and BMT fellowship.
Get to know our pediatric experts.

Michael Verneris, MD
Hematology/Oncology - Pediatric
Patient ratings and reviews are not available Why?


Hesham Eissa, MD
Hematology/Oncology - Pediatric, Pediatrics
Patient ratings and reviews are not available Why?

Would you like a second opinion?
Whether your child has a known diagnosis or you’re still looking for answers, our pediatric cancer and blood disorder specialists can help. We provide second opinions for many conditions so you can feel confident about your child’s treatment.
Request a second opinion from our Center for Cancer and Blood Disorders



 720-777-0123
720-777-0123




