- Doctors & Departments
-
Conditions & Advice
- Overview
- Conditions and Symptoms
- ¿Está enfermo su hijo?
- Parent Resources
- The Connection Journey
- Calma Un Bebé Que Llora
- Sports Articles
- Dosage Tables
- Baby Guide
-
Your Visit
- Overview
- Prepare for Your Visit
- Your Overnight Stay
- Send a Cheer Card
- Family and Patient Resources
- Patient Cost Estimate
- Insurance and Financial Resources
- Online Bill Pay
- Medical Records
- Política y procedimientos en el hospital
- Preguntamos Porque Nos Importa
-
Community
- Overview
- Addressing the Youth Mental Health Crisis
- Calendar of Events
- Child Health Advocacy
- Community Health
- Community Partners
- Corporate Relations
- Global Health
- Patient Advocacy
- Patient Stories
- Pediatric Affiliations
- Support Children’s Colorado
- Specialty Outreach Clinics
Your Support Matters
Upcoming Events
Mental Health Town Hall
martes, 23 de abril de 2024Join Children’s Hospital Colorado pediatric experts for a virtual...
-
Research & Innovation
- Overview
- Clinical Trials
- Q: Pediatric Health Advances
- Discoveries and Milestones
- Training and Internships
- Academic Affiliation
- Investigator Resources
- Funding Opportunities
- Center For Innovation
- Support Our Research
- Research Areas

It starts with a Q:
For the latest cutting-edge research, innovative collaborations and remarkable discoveries in child health, read stories from across all our areas of study in Q: Advances and Answers in Pediatric Health.


Orthopedics Education Videos
We care for patients’ growing muscles, joints and bones through sports medicine, surgery, rehabilitation and research.

At Children's Hospital Colorado, we're committed to providing the best care to patients with pediatric orthopedic conditions. Our team is constantly pushing boundaries to discover and implement the safest and most effective treatments.
In the videos below, our providers discuss how we’re advancing the field of orthopedics here in Colorado, across the country and around the world.
Dizziness after adolescent concussion
Dizziness is a common post-concussion symptom linked to poor sleep quality, postural instability and neck pain. New research from the Colorado Concussion Lab through Children’s Colorado delves into these connections, revealing how physical activity after a concussion may expedite recovery.
In this video, Kate Smulligan, PT, DPT, of the Sports Medicine Center at Children’s Colorado, shares the results of three research studies on the complexities of dizziness after adolescent concussion, offering new insights for providers on how varying intensities and dosages of physical activity post-concussion may influence recoveries and return to play timelines.
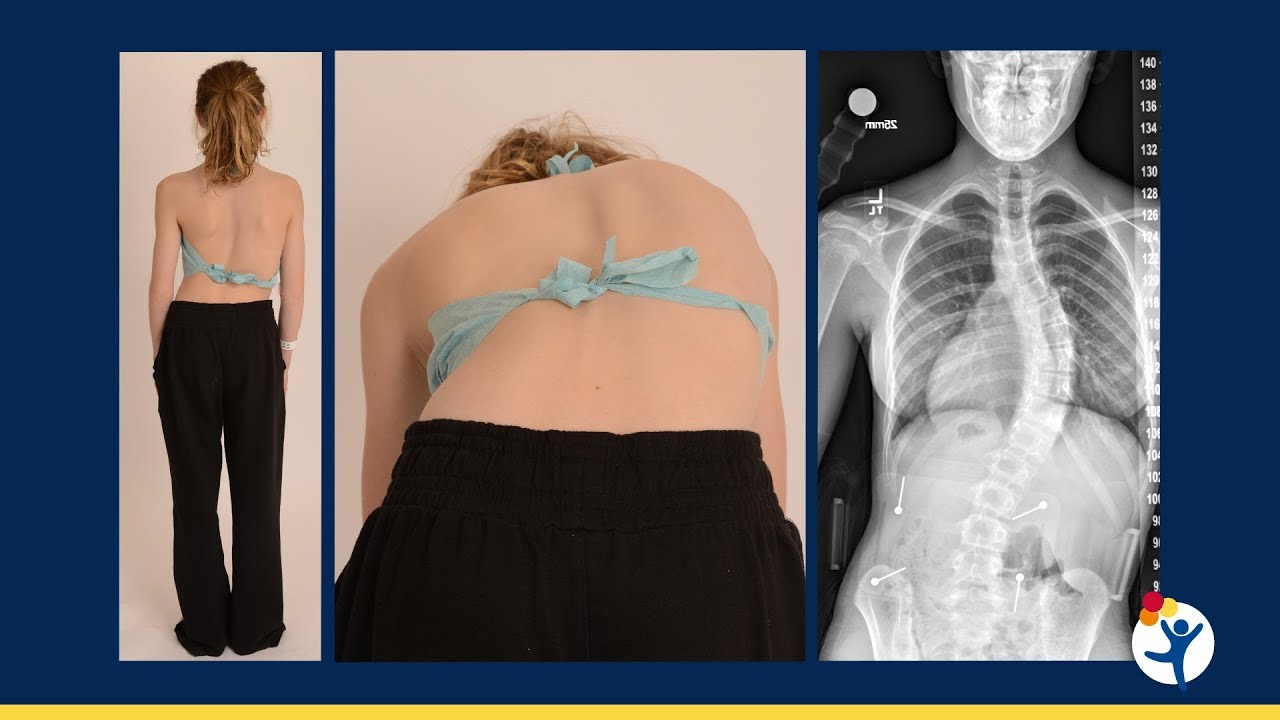
Pediatric scoliosis research
Pediatric scoliosis research focuses on understanding and improving the diagnosis, treatment and management of scoliosis in children and adolescents. This research covers various aspects of the condition, from the causes and risk factors to the impact on quality of life and the effectiveness of various treatment options. Advances in technology and medicine have created new optimism regarding research efforts aimed at understanding the cause of this complex pediatric condition.
Nancy Hadley-Miller, MD, of the Orthopedics Institute, and Patrick Carry, PhD, sat down to discuss the historical perspective of scoliosis and the current state of scoliosis research, including genetics, proteomics and the role of epigenetics in idiopathic scoliosis onset and progression.
Return to sports after posterior spine fusion for idiopathic scoliosis
Scoliosis is a curvature of the spine that measures greater than 10 degrees on an X-ray. While it’s concerning to learn a child has been diagnosed with scoliosis, most patients don’t require surgery. However, when curves are above 45 to 50 degrees, they’re likely to continue to worsen, leading to more back pain and worse outcomes. When patients receive surgical correction in adolescence, they can obtain better correction of their scoliosis with fewer complications and a much quicker recovery than adults.
In this video, Sumeet Garg, MD, answers questions that patients and families may have about how quickly their adolescent athletes can return to play after scoliosis surgery. Dr. Garg explains the guidelines for returning to sports and why patients at Children’s Hospital Colorado are able to recover from surgery so quickly –– thanks to shorter surgery times, reduced blood loss and very low rates of complications.
Neuromuscular hip dysplasia
Neuromuscular hip dysplasia is defined as a progressive subluxation of the hip joint and occurs when there is an imbalance of muscle tone around the hip joint. Although this condition is classically associated with a diagnosis of cerebral palsy (CP), there are many neuromuscular-like genetic, metabolic, and syndromic conditions that can create a similar appearance to that of a classic CP or spastic hip.
In this video, Sayan De, MD, explains how the pathophysiology of neuromuscular hip dysplasia differs from that of developmental hip dysplasia and the philosophy of a multidisciplinary care approach in a child with neuromuscular hip dysplasia.
Knee preservation: cartilage and meniscus injuries
The most common injuries among young athletes include tears or damage to the lateral and medial meniscus and knee joint cartilage. Conditions range from congenital disorders (e.g., discoid meniscus), joint disorders (e.g., osteochondritis dissecans) and traumatic injuries (e.g., patellar instability and ACL tears).
In this video, Curtis VandenBerg, MD, explains the importance of preserving knee cartilage and lateral and medial meniscus, and he shares emerging surgical techniques for treating common knee problems in young athletes. Since young athletes are different from adults, Dr. VandenBerg explains his nuanced approach to treatment and care.
Optimizing physical therapy and leveraging technology for athlete injury recovery
Physical therapy is an important component of recovery for young athletes after surgeries like ACL reconstruction, meniscus repair, patella stabilization and arthroscopic cartilage repair. But for young athletes with busy social and school lives, completing physical therapy isn’t always easy.
In this video, Curtis VandenBerg, MD, shares strategies for ensuring that young athletes have the resources they need to adhere to prescriptive physical therapy regimens and optimize a full recovery. Dr. VandenBerg and his team of experts also leverage technology, such as Children’s Hospital Colorado’s motion analysis lab, to identify biomechanical deficiencies throughout the recovery process.
The Running Athlete Clinic (TRAC)
Runners are often very motivated athletes, but many deal with an injury at some point, such as stress fractures, anterior knee pain, or iliotibial band syndrome. While there’s a plethora of resources for overcoming injuries and staying healthy, there’s also a lot of conflicting information, and it’s mostly geared toward adult athletes. Because pediatric athletes are different, the Orthopedics Institute at Children’s Hospital Colorado developed TRAC — a multidisciplinary clinic to help runners and other athletes in running-heavy sports (e.g., soccer, football, lacrosse and basketball) get back on track.
In this video, our multidisciplinary team of experts provides an overview of TRAC, a clinic that offers comprehensive and evidence-based medical, nutrition and rehabilitation care for pediatric running injuries and performance. When youth athletes come to TRAC, they can expect one-on-one consultations with a sports medicine doctor, sports dietitian and sports physical therapist. Their visit will often include a thorough medical and injury evaluation, imaging and lab work if indicated, nutrition consultation and running gait analysis. The team then designs an individualized treatment plan that includes cross-training, physical therapy and a return-to-run plan.
Surgical innovation and robot-assisted pediatric spine surgery
The use of robotic-assisted surgical procedures in pediatrics has been on the rise. Early adoption of this technology has spurred innovation, most recently in the field of spine surgery. The accuracy of robotic systems allows for greater fixation through precise placements of large screws into small pedicles of the spine.
In this video, Mark Erickson, MD, shares what he has learned after completing more than 300 robotic-assisted pediatric spine surgical procedures. Dr. Erickson offers advice for surgeons interested in bringing robotics innovation into their institution.
Chronic recurrent multifocal osteomyelitis (CRMO): Diagnosis and treatment pathways
CRMO is an autoinflammatory bone disorder that almost exclusively affects the skeletally immature –– children and adolescents. CRMO often resolves once they reach skeletally maturity. Since CRMO is a diagnosis of exclusion, biopsies, MRIs and genetic testing are often needed to rule out more serious causes of symptoms (e.g., bone pain, weakness, weight loss), such as leukemia, lymphoma, bacterial osteomyelitis, Ewing sarcoma and Langerhans cell histiocytosis.
In this video, Associate Professor of Orthopedic Surgery Nathan Donaldson, DO, discusses the use of radiographs and MRIs for imaging and the importance of biopsies to confirm CRMO diagnosis. CRMO treatment options include NSAIDs, methotrexate, TNF inhibitors or biphosphanates with a goal of being pain-free for 6 months prior to stopping treatment.
Total joint arthroplasty before 25
Total hip arthroplasty and total knee arthroplasty are becoming more common in younger patients as a last resort when conservative care has failed, pain is no longer tolerable and joint preservation is not an option. While there are a variety of diagnoses leading to arthroplasties, such as avascular necrosis from leukemia or rheumatologic disease treatments, pain mitigation options (e.g., weight management, physical therapy, activity modification) are utilized before arthroplasty. Patients receiving a TJA have comparable mental and physical function compared to their peers.
In this video, Nathan Donaldson, DO, discusses when a TJA should be utilized, common conditions leading to TJA, pain management options and outcomes –– including patient-reported quality of life and function.
Infant hip dysplasia
Hip dysplasia in infants occurs when the hip bone and socket are not formed properly –– ranging from minor looseness in one or both of their hip joints to complete dislocation. While infant hip dysplasia can be resolved with a Pavlik harness or rhino hip abduction brace, even mild hip dysplasia can cause problems in adulthood, such as arthritis or hip replacement.
In this video, Margaret Siobhan Murphy-Zane, MD, discusses the causes of infant hip dysplasia (e.g., breech positioning during birth, tight swaddling), standard treatments and the importance of diagnosing within the first few months of life. Normally, pediatricians refer patients for ultrasounds at 6 weeks of age, unless they suspect the hip is dislocated.
Innovations in orthopedic surgery
Advances in technology are changing the world, and that’s especially true for orthopedic surgery. Our orthopedics team is using innovations like our animation studio, 3D printing and robotics to make surgery safer for patients.
In this video, pediatric orthopedic surgeon Mark Erickson, MD, explains how we’re applying these advancements to provider training, patient education and the operating room. Learn how we’re using technology to improve orthopedic care.
Reducing blood loss during scoliosis surgery
The Children’s Colorado Spine Program team performs more than 200 spine procedures annually, including approximately 100 procedures for adolescent idiopathic scoliosis. Despite excellent clinical outcomes, our spine team began a focused effort in 2013 to reduce blood loss during scoliosis surgery.
In this video, pediatric orthopedic surgeon Sumeet Garg, MD, discusses the systematic quality improvement approach that our spine team has implemented to dramatically reduce blood loss and nearly eliminate the need for blood transfusion during corrective surgery for adolescent idiopathic scoliosis. Learn how we’re making scoliosis surgery safer for pediatric patients.
Decreasing anterior cruciate ligament (ACL) re-tear rates in young athletes
Our Sports Medicine team is leading the way in pediatric ACL repair and reconstruction surgeries by using the most proven methods for pediatric athletes.
In this video, Surgical Director of Sports Medicine Jay Albright, MD, explains the techniques he uses to repair and reconstruct ACLs in young athletes. Watch to learn how we’re lowering re-tear rates and helping more athletes return to sport safely.
Advancing Pediatric Concussion Care through Research
Our team at the Concussion Program specializes in the evaluation and treatment of children and adolescents who have experienced a concussion. In this video, pediatric sports medicine physician and co-director of the Concussion Program, Julie Wilson, MD, discusses multiple areas of concussion research focused on clinical outcomes for our patients. Watch the video to learn about the impact of neck pain and sleep problems on concussion symptoms, as well as recovery predictors and the role of physical activity in concussion management.
Duchenne Muscular Dystrophy Primary Care Guidelines
Thanks to FDA approved treatments and novel clinical trials, care for boys with Duchenne muscular dystrophy has greatly improved. However, because there is still no cure, it is critical that care providers optimize medical management through close monitoring and early interventions.
In this video, Susan Apkon, MD, co-director of our Neuromuscular Program, shares her expertise regarding the management of boys and young men with Duchenne muscular dystrophy in the primary care setting. Watch the video to learn the general health guidelines and a discussion of different acute problems care providers may encounter in the primary care setting.



 720-777-0123
720-777-0123