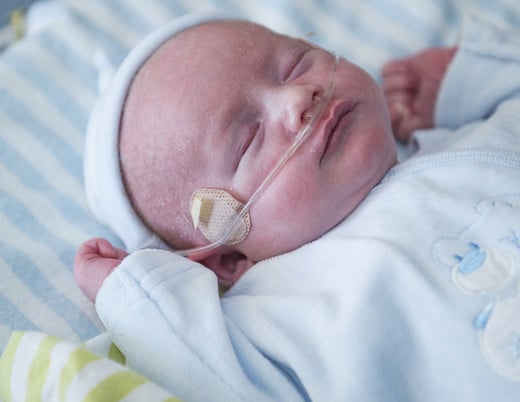
Kylie Tatro has worn a nasal cannula her entire life. She needs the help drawing oxygen into her blood. Like nearly half of kids with Down syndrome, Kylie has pulmonary hypertension. Like many more, she also has a heart defect.
Pulmonary hypertension in children with Down syndrome
Both her pulmonary hypertension and her heart defect put Kylie at risk for hypoxic brain damage. Heightening Kylie's risk even further is her Moyamoya disease — a rare condition that constricts the blood vessels in her brain. She also aspirates fluids.
And that's just during the day.
"We're a mobile hospital," says Beau, Kylie's father. "Every time we go out, we take along a nebulizer, a suction machine, thickened fluids, oxygen. If we're going to be gone long enough, we'll load up the oxygen concentrator."
At night, Kylie struggles with sleep apnea. Typically, the treatment for that is a continuous positive airway pressure machine, or CPAP, which seals the nose with a mask in order to force air into the airway manually. Kylie was 5 years old when she got her first one. She hated it.
"She'd take it off constantly during the night," says Stephanie, her mother. "We'd be up all the time. The monitors would start beeping, and we'd get up again."
"We even tried putting her cannula on underneath the mask, hoping that might help her oxygen levels," adds Beau.
It didn't. Meanwhile, Kylie's repeated low blood-oxygen was making her pulmonary hypertension worse. That, in turn, was putting more strain on her already strained heart.
Every night, Kylie's condition was deteriorating.
The problem with CPAP for children
Breathing Institute pulmonologist and sleep medicine physician Stephen Hawkins, MD, pulls an unwrapped CPAP apparatus off a shelf in a supply room. The box features a gray-haired man smiling beneath the mask attached to his face.
Dr. Hawkins nods toward the remaining rows of CPAP boxes, all similarly arrayed.
"As you can see, these are marketed pretty much exclusively to middle-aged dudes," he says. "There aren't any really great options for little kids."
For kids, the masks are cumbersome, uncomfortable. They don't fit right. Even when kids do tolerate the mask, the nightly pressure over time can have a deforming effect on growing facial bones.
Sleep apnea and Down syndrome
Nationally, 60% of kids with Down syndrome show abnormal sleep studies by 4 years old. The Sleep Center team at Children's Colorado found that the number at Denver's altitude was closer to 80%.
"A lot of it is mechanical," says Francis Hickey, MD, FAAP, Medical Director of the Anna and John J. Sie Center for Down Syndrome at Children's Colorado. "These kids have smaller airways, bigger tonsils, smaller mouths with relatively bigger tongues. It's harder to get the air where it needs to go."
The problem is even worse for the 50% of kids with Down syndrome accompanied by pulmonary hypertension, which sleep apnea can both cause and aggravate. Animal studies have shown that even brief, regular interludes of low blood oxygen can lead to pulmonary hypertension.
"In Denver, we tend to see more pulmonary hypertension in kids with Down syndrome than they see in the rest of the country," remarks pediatric cardiologist Dunbar Ivy, MD, one of the nation's top experts on pulmonary hypertension, and one of several experts involved in Kylie's care at Children's Colorado. "They also tend to have some reflux and aspiration, which just sets them up for further inflammation of the lungs."
CPAP as a last resort
Although Kylie lives in Wichita, Kansas, and thus didn't have altitude to worry about, her particular combination of complications made her case especially severe.
"She was to the point where, if her pressures got any worse, we'd have to try a valve repair," says Dr. Hickey. "And there was a good chance there would be complications."
"The thing is, by the time we recommend CPAP, we've already tried every other means we've got," adds Dr. Hawkins. "Taking out the tonsils and adenoids, using nasal medications — anything we can do to open the airway. So if it doesn't work, we try more medications and more operations, and the process starts all over again."
"She just could not get used to that mask," says Beau. "But she was used to wearing the cannula all day long. We were asking if she could get some kind of cannula-type assistance, if there even was something like that in existence."
There wasn't just yet — but the same thought had occurred to Children's Colorado pulmonologist Ann Halbower, MD, one of the nation's top pediatric sleep experts.
Harnessing AIRVO for sleep apnea
A CPAP machine needs a seal to push air into the lungs. A cannula can't create that seal — but if the airflow was great enough, Dr. Halbower speculated, maybe when it hit the back of the nasal passage it would stimulate those muscles to keep the airway open on their own.
She and her team had already experimented with a makeshift machine of their own design when the AIRVO debuted. Designed for adults suffering from chronic obstructive pulmonary disease, the AIRVO pushes air through a cannula at a rate of roughly 15 to 40 liters per minute — about 20 times the airflow of a regular cannula. Perhaps more importantly, it heats and humidifies the air before it does.
"The design itself is not all that revolutionary," says Dr. Hawkins, Kylie's primary sleep doctor. "It makes comfortable, refreshing air, instead of the cold, dry air that typically comes out of a cannula, and it pushes a lot of it. The novel thing is applying it to these kids."
Kylie was one of 10 kids that doctors Halbower and Hickey initially studied — the first pediatric patients to use the device. It worked. Kylie's blood-oxygen saturations substantially increased. She slept better. Her heart improved.
"It probably saved her life," Dr. Hickey says.
A new option for kids who can't tolerate CPAP
Kylie's example is extreme, but thousands of kids around the nation stand to benefit. At Children's Colorado alone, more than half of the kids the Sleep Center sees for apnea can't tolerate CPAP. Not all of them would benefit from AIRVO — since Kylie's study, the team has found it doesn't work for everyone — but many of them would. That's especially true for infants and toddlers, whose faces are too small for CPAP masks.
"Many of these kids did even better than we thought they would," says respiratory therapist Kathy Simar, RRT, RPSGT, who runs the AIRVO studies. "I think this could have many more uses than what we're doing now."
Kylie's care at the Sie Center
Now 12 years old, Kylie is one of the AIRVO's longest-standing pediatric patients, and she's still doing well. She has more energy. She gets sick less often. She hasn't had an unscheduled hospital stay in two years. With all that spare time, she likes playing with her "flippy," a homemade toy she fashions from a ribbon or strip of newspaper tied to a pencil — but she spends even more time being active. She rides horses and a three-wheeled bike. With some help from a 50-foot oxygen cord tied to her wrist, she dances ballet. She runs. A lot.
That's largely possible because of the backpack she now wears to carry her oxygen tanks, suggested last year at the Sie Center by Dr. Ivy. The setup allows her more independence and freedom of movement than she's ever enjoyed before.
"She loves it," says Stephanie. "We went to a cousin's wedding, and she was on cloud nine. She could run around and dance all she wanted."
"As far as our routine, it was just a normal burden that went away," notes Beau. "The two of us could never really enjoy family gatherings. We'd worry about all these people not used to being around an oxygen cord, so we'd spend the whole outing running around making sure it wasn't tripping anybody."
What Kylie can do
Kylie has a lot going for her. She's mobile. She can feed herself. She can read a book. With her basic needs taken care of, she can realize her full potential, and her family has a lot of hope. They're not the only ones.
"Dr. Hickey always says, 'Oh, she's going to hold a job. She's going to do well. She's going to amaze you, how much she can do,'" says Beau. "There's always been such a positive outlook for her. So we're just trying not to limit her. We want to give her all the options and see what she can do."
Featured Researchers

Stephen Hawkins, MD
Pediatric sleep specialist
The Breathing Institute
Children's Hospital Colorado
Associate professor
Pediatrics-Pulmonary Medicine
University of Colorado School of Medicine

Francis Hickey, MD, FAAP
Medical Director
The Anna and John J. Sie Center for Down Syndrome
Children’s Hospital Colorado
Professor
Pediatrics-Linda Crnic Institute for Down Syndrome
University of Colorado School of Medicine





 720-777-0123
720-777-0123