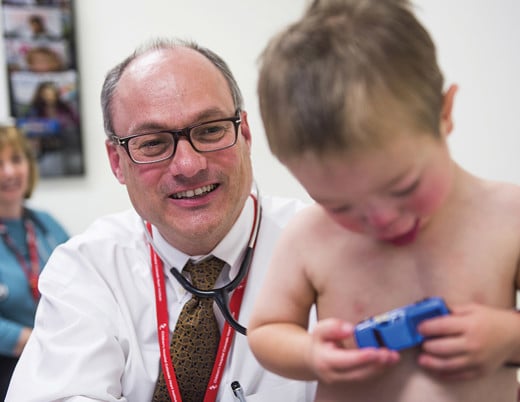
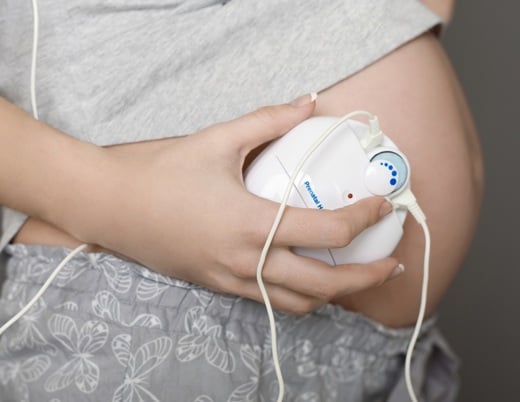
Maria got the diagnosis at her 20-week ultrasound: Her baby, Calista, had hypoplastic left heart syndrome, or HLHS. As an emergency department nurse in Greeley, Colorado, Maria had an idea of what that meant. What she didn’t know, she got right to work finding out. It didn’t take her long to hone in on stem cells.
Kids with HLHS face a grim prognosis. The right ventricle, normally responsible only for pulmonary circulation, has to pump blood through the entire body on its own. And the trifecta of HLHS surgeries that reconfigure the circulation to make that possible, while lifesaving, don’t happen without scarring. Scarring, in turn, further weakens the myocardium.
"We don't know yet if we can make kids with single ventricle disease live longer, but we think heart function can be improved by the injection of stem cells," says James Jaggers, MD, Chief of Pediatric Cardiothoracic Surgery at Children's Colorado's Heart Institute.
Stem cells don't survive in myocardial tissue, but they do secrete substances that can attract other cells to strengthen and possibly replace damaged heart muscle cells.
That research, and research like it, drives the mission of the Mayo Clinic's HLHS consortium, a multi-institutional group now harvesting patients' own umbilical cells at birth to inject back into their hearts during staged reconstruction. Through such injections, cardiothoracic surgeons like Dr. Jaggers hope to minimize scarring and promote regeneration in areas affected by surgery — maybe even strengthen the right ventricle and help it function like the left.
"The important thing is the power of multiple heart programs all working toward the same goal."
- JAMES JAGGERS, MD
"We had the entire team present at Calista's delivery for a seamless transition to neonatology," says Michael Zaretsky, MD, Medical Director of the Colorado Fetal Care Center. "Our fetal cardiology team harvested the cord blood."
Calista got some of it back during her Glenn procedure last year. For now, there's no way to know if it will help. But it's an important first step.
"If it doesn't help Calista," says Maria, "I hope this work will help other kids down the road."
Featured Researchers

James Jaggers, MD
Co-Medical Director, Heart Institute
Children's Hospital Colorado
Barton-Elliman Chair in Pediatric Cardiothoracic Surgery, Surgery-Cardiothoracic
University of Colorado School of Medicine

Michael Zaretsky, MD
Director of Research
Colorado Fetal Care Center
Children's Hospital Colorado
Professor
OB-GYN-Maternal Fetal Medicine
University of Colorado School of Medicine





 720-777-0123
720-777-0123