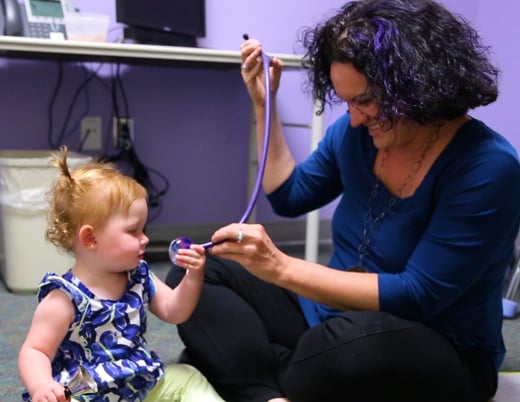
Lucy Washburn was a fussy baby. For new parents Cynthia and Brad Washburn, that didn't seem unusual. That's just what kind of baby Lucy was. But when Cynthia noticed at 3 months what looked like a hernia around Lucy's groin, she decided to take her to the pediatrician near their home in Winter Park, Colorado, nestled into the mountains west of Denver at about 9,500 feet.
"They drew blood," says Brad, "and it all just exploded from there."
An hour later, Lucy was in a helicopter rushing to Children's Hospital Colorado while her parents drove down behind.
"She had rip-roaring high blood pressure," says Chief of Pediatric Nephrology Jens Goebel, MD, who managed her care. "It took astronomical amounts of blood pressure medications to get it under control."
Excessive protein in her urine prompted an initial diagnosis of congenital nephrotic syndrome, but a genetic test came back unrevealing. Her enlarged kidneys and high blood pressure, for a while, led to speculation she might have polycystic kidney disease. But that genetic test, too, came back negative.
"They went through four or five diagnoses," says Brad.
"And God knows how many genetic tests," Cynthia adds. "They just didn't know what the cause was."
The clue that pulled it all together
It was a frightening ordeal, particularly for Cynthia, who, as a teen, had suffered a meningococcal infection that came on suddenly, shut down her major organs and put her in a coma that lasted weeks. It left her with skin grafts all over her body. Doctors were forced to amputate her legs.
"My mom flew out from Australia when Lucy was in the hospital," Cynthia recalls. "She was saying, 'it's just like déjà vu.'"
Lucy's condition stayed distressingly touch-and-go for three months. Her team assigned her the umbrella diagnosis of chronic kidney disease, though they still didn't know exactly what. But once she was stable, they sent her home.
And for more than a year, she did alright — well enough for her team to gradually reduce her meds. Cynthia and Brad settled into the routine of bringing her in for blood work once a month.
"She started to become anemic, and that anemia became more progressive," says pediatric nephrologist Bradley Dixon, MD. "That's not unusual for chronic kidney disease. But her kidney function was about 70% of normal, and the anemia was way out of proportion to that."
Then, in April of last year, a routine blood test showed Lucy's platelet count rapidly dropping.
That was the clue that pulled it altogether.
"It's like a Ferrari someone cut the brakes on. As long as it sits in the garage, it's alright. But if you take that out at 150 mph and you don't have brakes, bad things are going to happen."
- BRADLEY DIXON, MD
How the complement system affects the kidneys
Drs. Goebel and Dixon agreed: The most likely culprit was in fact a blood disease, thrombotic microangiopathy, or TMA. It results when platelets clump and plug up networks of capillaries — such as those of the kidneys — deforming red blood cells as they squeeze through. Hence the high blood pressure. Hence the anemia. Hence the low platelet count.
TMA has many causes, from E. coli to cancer. In Lucy's case, Drs. Dixon and Goebel suspected it was atypical hemolytic uremic syndrome, or aHUS, the result of a genetic defect in a component of the immune system known as complement.
"Certain molecules on the surface of bacteria don't occur on human cells," says Dr. Dixon. "These innate parts of the immune system can recognize danger patterns and go after a pathogen without ever being exposed to it."
Complement destroys the bacterium meningococcus by punching a hole in its cell wall. Its power is immediate and immense. And once it's triggered, it requires a strong regulatory response. In aHUS, that doesn't happen.
"Complement is a protein cascade," says University of Colorado School of Medicine immunologist Ashley Frazer-Abel, PhD, one of the nation's foremost experts on complement proteins. "These proteins exist in circulation, and in an activating event like an infection, it's a cycle of self-perpetuation. It's very good locally to fight infection, but when it's systemic or uncontrolled, it's doing direct damage to the body or recruiting other immune cells to perpetuate that damage."
"It's like a Ferrari someone cut the brakes on," says Dr. Dixon. "As long as it sits in the garage, it's alright. But if you take that out at 150 mph and you don't have brakes, bad things are going to happen."
Blocking the immune power of the complement system
That's what was happening to Lucy, and the complement system's sudden spiral led to another 7 weeks in the hospital. Still, with a diagnosis also came the brake Lucy needed: powerful complement-blocking agents that hobble proteins in the chain.
That would save her life, but it would also leave her complement system powerless against meningococcal disease — the same infection that had taken Cynthia's legs.
"That was a difficult conversation to have," says Dr. Dixon. He speculated it was possible that the same underlying defect had caused Cynthia's infection. Perhaps a defective complement system depleted by its own autoimmune attack had left her vulnerable to the infection in the first place.
The other downside was that complement-blockers required infusion — a long day for the Washburns, who would have to drive a nearly 150-mile round trip. Drs. Goebel and Dixon already had a patient enrolled in a clinical trial for an experimental, extended release complement-blocking drug, which would only require Lucy to come in monthly. Her condition was so rare that, once she entered the trial, Children's Colorado became one of just two sites in the world with more than one patient enrolled.
Weighing the diagnosis of aHUS
Initially it worked. Lucy's platelet count went up and her blood pressure stabilized. But by the next week, a lab check between infusions caught her platelet count dropping and anemia setting in.
Drs. Dixon and Goebel, who number among the world's foremost experts in treating TMA in children, considered the possibility that they'd misdiagnosed. Still, they had experience enough to feel confident they'd got it right.
They also knew that dosing regimens in clinical trials like the one Lucy was in tend to extrapolate dosing regimens from adults. But young children metabolize some drugs much faster than adults and older children. The half-life is shorter. Their team had studied that phenomenon and published their results. Maybe the experimental drug had just worn off.
The real question, they surmised, was whether the complement system was blocked.
There was only one real way to find out: an exacting version of a test called CH50. It's the most sensitive measure of complement — and the one most difficult to perform. Because of the difficulty, it can take weeks to get results. Only a handful of labs in the country offer it.
One of them belongs to Dr. Frazer-Abel: Exsera BioLabs, just across the street from Children's Colorado on the Anschutz Medical Campus.
Bursting blood cells: how CH50 works
A few tests measure complement system activity, but none are as sensitive or accurate as CH50. It's also the most difficult to perform, because it involves living cells.
"Basically, you take sheep red blood cells and decorate them with antibodies that prime them for killing by complement," says Dr. Dixon. "Then you dump in patient serum and if there's active complement, it will punch holes in these cells. That releases hemoglobin, which is a pigment, so then you measure the color."
"You can actually see it," adds Dr. Frazer-Abel.
Historically used to measure complement in the opposite direction — in the case of recurrent bacterial meningitis, say — CH50 has been around for nearly 100 years. But it's not easy to pull off.
"Since they're live cells, they're more complex to work with than a purified reagent you just pull off the shelf," says Dr. Frazer-Abel. "It's also more realistic, because our bodies are made of cells. A sheep can get sick. You have to be able to control for that. So it takes a lab that knows what they're doing."
It's also far from the only complement test Exsera — one of the only labs in the nation dedicated exclusively to complement — performs. There are 56 proteins in the complement system, says Dr. Frazer-Abel. Exsera measures almost all of them.
"We're friends with Exsera," says Dr. Goebel. "We can draw blood in the morning and get a result by sunset."
The right (but risky) choice
The result proved what Drs. Dixon and Goebel suspected: complement wasn't blocked. The trial drug wasn't enough to suppress Lucy's complement system through the month, and because the drug was experimental, there was no way to know if they could safely adjust the amount or frequency of the dose.
They also knew that a drug already on the market called eculizumab, though it would require more frequent infusions, would do the job.
"The recommended dosing of these complement-blocking agents is, in Dr. Dixon's and my experience, not sufficient for children with rare variants of this disease," Dr. Goebel says. "We've seen it repeatedly and often enough that we don't blink anymore when we say we need to treat this child more aggressively."
"At the end of the day, we pulled her out of the study," says Dr. Dixon.
It took courage and a sure hand — but it worked. On a high dose of eculizumab every two weeks, Lucy's condition stabilized. A genetic test eventually confirmed the diagnosis. With vaccinations against meningococcus and prophylactic antibiotics, along with several blood pressure medications, Lucy lives the life of a relatively normal 2-year-old.
It's not perfect, but it's much better than the alternative. It wasn't so long ago, after all, that aHUS wasn't often diagnosed. Kids went through fruitless kidney transplants, sometimes several, to no avail. For now, Lucy's team is working with a health center near Winter Park to try to move Lucy's bi-weekly infusions closer to home.
As it stands, that's the best and only option, perhaps for the rest of Lucy's life.
"We've seen it repeatedly and often enough that we don't blink anymore when we say we need to treat this child more aggressively."
- JENS GOEBEL, MD
Decoding the genetics of complement factor H
But there's hope the work of complement researchers like Drs. Dixon and Frazer-Abel may change that one day. Currently, they're working with the Molecular Genetics Lab at Children's Colorado to understand the functional consequences of mutations in complement factor H, the group of genes that governs complement's braking system.
"That's the final piece we need for our existing arsenal," says Dr. Frazer-Abel. "We're realistically only five or six months out."
Still, it won't be easy, says microbiologist Alisa Gaskell, PhD, Scientific Director of the Molecular Genetics Lab at Children's Colorado. In fact, in many ways, it will require radically revising the standard practice of gene sequencing.
"First generation sequencing was akin to reading long stretches of DNA kind of like you read a book," she says. "We've since developed new technologies where they chop the book into single words, then we amplify those words, and a computer program rearranges them back into order and gives a report — basically the Cliff's Notes."
It's a much faster method. The Human Genome Project took just under 13 years to complete. The current record, completed at The Institute for Genomic Medicine in San Diego, is 19 hours.
But the current method is a problem when analyzing genes like those of complement factor H, which closely resembles five other genes. Sequestering and ferreting out the meaning of tiny changes that lead to protein malfunctions depends on context. The conventional method can't carry that kind of context.
"We're looking at it differently," says Dr. Gaskell. "We're saying, 'How can we, within these constraints, leave sort of cookie crumbs that give us clues to the sequence. We're basically breaking with doctrine."
A new method of genetic sequencing
Essentially, Dr. Gaskell and her team are changing the way they break up the DNA, a method that involves overlapping longer strands of code.
On the wet lab side, where the DNA is extracted, that means using more mature enzymes that will read a longer stretch of code without error. On the dry lab side, where the DNA is processed, it's writing new algorithms that can not only arrange those stretches, but accurately flag where something might have gone wrong.
"It's reengineering both those components in a unified way that will get us to the point where we're only looking at words that come from this gene and nothing else," says Dr. Gaskell. "It will take us a few cycles, but once we get to where we can resolve a sentence, we can start pressing clinical samples through and doing blinded studies that compare what we find to clinical results. Then we'll see if we have a system that works."
A day at a time
"We have about an acre of property," Brad remarks, watching Lucy zip around on a strider. "She knows every inch of it."
He and Cynthia, both of whom work as ski instructors for the National Sports Center for the Disabled, plan to take her down the bunny hills in a backpack this year. They'll wait until she's 3 to put her on skis.
"She's doing great. She really is," says Cynthia. "She's at home with me four days a week and goes to day care one day. She likes the social part, but I guess we're still a bit terrified of the infection piece. Maybe a little bit further down the track, we could push it to two or three days. But right now one day a week is as much as I can put up with."
In the meantime, they're taking it one day at a time.
"We're stronger just knowing there's a treatment," says Cynthia. "Lucy's team is amazing. We trust them with her life completely."
Featured Researchers

Bradley Dixon, MD
Department Chair
Pediatric Nephrology
Children's Hospital Colorado
Associate professor
Pediatrics-Nephrology
University of Colorado School of Medicine

Ashley Frazer-Abel, PhD
Assistant research professor
Medicine-Rheumatology
University of Colorado School of Medicine

Alisa Gaskell, PhD
Scientific Director
Precision Medicine Institute
Children's Hospital Colorado





 720-777-0123
720-777-0123