Key takeaways
-
Our researchers studied loss of control eating in obese teens before bariatric surgery and up to four years after bariatric surgery.
-
They found that loss of control in eating in patients was associated with decreased long-term BMI change and increased weight gain.
-
They also found that loss of control eating decreased before surgery and in the first six months following surgery, but increased four years after surgery.
Research background: Loss of control eating before and after teen bariatric surgery
Bariatric surgery is becoming more popular for the long-term treatment of severely obese teens. Common eating behaviors, including loss of control eating (LOC), can undermine surgical outcomes. Loss of control eating is the feeling that you cannot control what or how much you eat. There is a strong association with loss of control eating and weight gain. LOC also points to serious psychosocial complications.
Study authors previously reported that nearly 30% of teens seeking bariatric surgery experienced loss of control eating prior to surgery. However, there is very little information about its long-term course and impact on weight outcomes.
Study authors aimed to extend their previous research on presurgical loss of control eating among severely obese teens by investigating the course and outcome of loss of control eating from presurgery through a four-year follow-up.
Research methods: Teen-Longitudinal Assessment of Bariatric Surgery cohort data used in study

- Initial health assessment: within 30 days of surgery
- Postsurgical follow-up at: six months, one year, two years, three years and four years
Two types of loss of control eating were examined via a questionnaire:
1. Loss of control eating while consuming an unusually large amount of food (objective binge eating; LOC-OBE)
2. Loss of control while eating continuously (continuous loss of control eating eating; LOC-C)
Research results: Presurgery and postsurgery loss of control eating
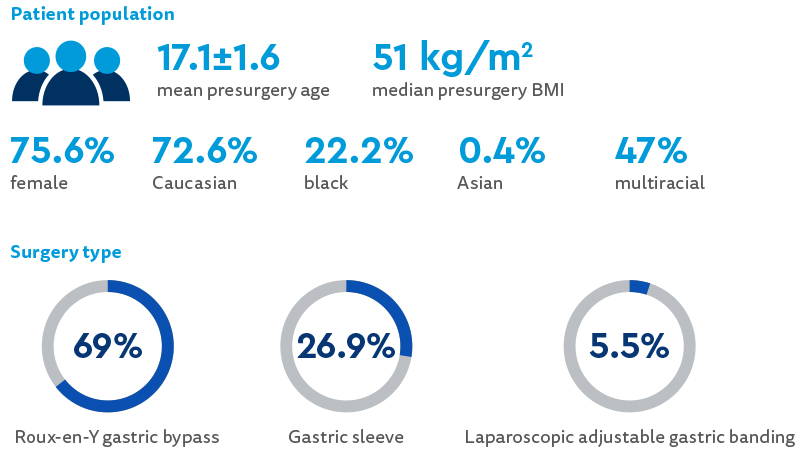
At baseline, objectively large loss of control eating was reported by 15.4% of participants and continuous loss of control eating was reported by 27.8% of participants. Both forms of loss of control eating were significantly lower at all five postsurgical follow-up visits compared with presurgery (all p<.001).
Both behaviors gradually increased from six-month to four-year follow-up (ps<.05), but presurgical loss of control eating did not impact the percentage of BMI change over follow-up (p=0.72). However, study authors found that loss of control eating at one-, two- and three-year follow-up was associated with a lower percent BMI change at the next consecutive assessment (ps<.05).
Research discussion: Loss of control eating and weight loss maintenance after teen bariatric surgery
Study authors observed a dramatic decrease in the occurrence of LOC eating in the period immediately after surgery, followed by gradual increases of loss of control eating over four years of postoperative follow-up.
The reporting of loss of control eating at presurgery and six-month follow-up was not predictive of later weight change, but loss of control eating at one-, two- or three-year follow-up predicted greater weight regain for teen patients. The findings indicated that loss of control eating while eating continuously is more common than binge eating after bariatric surgery.
The current study findings also contradict previous findings in teens by showing that presurgical loss of control eating had no real impact on the postsurgical BMI percentage change. However, the current study findings are consistent with most adult findings.
Research conclusions: Managing loss of control eating for long-term outcomes
The study found that the rate of loss of control eating decreased from presurgery to six-months postsurgery, but increased four years after surgery. Presurgical loss of control eating had minimal impact on weight outcomes and should not preclude surgical treatment.
However, clinicians should assess and work with teen patients to manage and monitor loss of control eating in the four years after surgery since it can adversely affect long-term weight outcomes.





 720-777-0123
720-777-0123