Key takeaways
-
Our researchers studied ERAS protocols in pediatric urology patients undergoing reconstructive surgeries including bowel anastomosis.
-
When compared to a control group, they have so far found that the ERAS patients had better outcomes including length of stay and decreased readmissions.
-
Our researchers have begun a larger, multicenter study to confirm the benefits of adopting the ERAS protocol for pediatric patients, expanding study criteria to include continent urinary diversion and concomitant bladder neck procedures.
Research background: Enhanced Recovery After Surgery protocols need further exploration in pediatric urology
The Enhanced Recovery After Surgery (ERAS) Society established guidelines for adult patients recovering from a variety of surgeries. ERAS goals include:
- Maximize pain control
- Minimize perioperative metabolic stress
- Optimize fluid balance
- Decrease convalescence time
In adult patients, the protocols led to decreased length of stay and lower perioperative complication rates without related increases in hospital admissions. While recovery protocols have helped adult surgical patients, only a few reports detail ERAS protocols being applied to pediatric surgeries, and none to pediatric urology surgeries.
Researchers in the Department of Pediatric Urology at Children's Hospital Colorado sought to determine if an ERAS protocol would be safe and effective for children undergoing urologic reconstructive surgeries. Seeing positive results in an initial pilot, they have since expanded the study to include multiple centers, including:
- St. Louis Children's Hospital
- Ann & Robert H. Lurie Children's Hospital of Chicago
- Children's Hospital of Pittsburgh
- Cincinnati Children's Hospital
- Children's Hospital of Richmond at VCU
Research methods: Researchers studied pediatric reconstructive urology patients using select adult ERAS protocols
The study authors initially targeted patients under the age of 18 who had a urologic surgery that included a bowel anastomosis (such as bladder augmentation or continent ileo-vesicostomy). They selected 16 adult ERAS protocols to define and implement with enrolled patients spanning the pre-operative, intra-operative and postoperative phases of care.
Since then, they've expanded the study to include 20 ERAS protocol process measures, covering procedures such as continent urinary diversion and concomitant bladder neck procedures, and patients up to age 25.
Preoperative protocols:
- Provide preoperative counseling on ERAS protocol and expectations for recovery, pain control and diet
- Administer a preoperative clear liquid carbohydrate load up to two hours prior to surgery
- Encourage patients to eat a regular diet the night before surgery
- Minimize time nil per os
- Avoid hyperosmolar bowel preparation; instruct patients on a bowel regimen that should be continued up to the night before surgery
- Give guideline-appropriate antibiotics within 60 minutes prior to incision
Intraoperative protocols:
- Use regional anesthesia
- Avoid excess drains
- Maintain euvolemia
- No opioids
- Minimally invasive assistance
Postoperative protocols:
- Avoid postoperative nasogastric (NG) tube on leaving the operating room
- Provide nausea and vomiting pharmacologic prophylaxis
- Provide early enteral feeding with clear liquid diet on the evening of surgery and regular diet on the day after surgery
- Encourage early mobilization
- Use non-opioid analgesics and avoid opioids
- Discontinue maintenance intravenous fluids by postoperative day two
The anesthesia team developed a detailed intraoperative protocol to help maximize adherence. The urology team set a preoperative carbohydrate load and stressed postoperative care plans at the end of the operative note in addition to direct discussions with the team.
Discharge criteria:
- Tolerate oral intake
- Have bowel function
- Return to baseline mobility
- Understand catheter-related instructions from a urology nurse
In the pilot study, the historical study control group included all pediatric patients in the five years before the implementation of the ERAS protocol who were under the age of 18 and underwent a surgery that included a bowel anastomosis.
Thirteen pediatric patients met the study criteria for inclusion and all participated; 26 patients were included as historical controls after propensity matching occurred. The expanded study will ultimately enroll 64 ERAS participants and 128 recent historical controls. About half are enrolled so far.
Research results and discussion: ERAS protocols improved care for pediatric reconstructive urology patients
In our pilot study, the median protocol score in the ERAS protocol group was 12/16 versus the median protocol score of 8/16 in the historical control group.
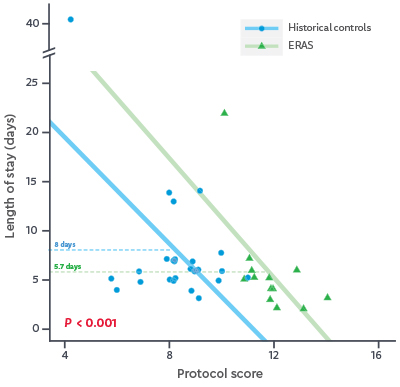
Protocol score for historical and ERAS patients plotted against length of stay (LOS). Increased scores were associated with decreased LOS. Solid lines represent linear regression models for each group. The two models were significantly different (P < 0.001).
In addition, the results included:
- Decrease in LOS from 8 days to 5.7 days
- Improved use of preoperative liquid load
- Intraoperative and postoperative opioids avoided
- Early discontinuation of IVF
- Early feeding
- Decreased 90-day complications from 2.1 to 1.3 per patient
Study authors found that the implementation of ERAS improved the consistency of care. The theories of ERAS appeared to drive improvements including maintenance of euvolemia by avoiding excess fluids, multimodal pain prevention and early feeding.
Research conclusion: ERAS protocols are safe in pediatric reconstructive urology patients; further study needed
Study authors found that ERAS is safe for pediatric patients who undergo reconstructive operations requiring bowel anastomosis. A multicenter study expanding inclusion criteria, procedures and protocols is underway. Authors will also study whether cost-effectiveness of postsurgical outcomes improves through the use of ERAS protocols.
See more about the expanded, prospective multicenter ERAS study at ClinicalTrials.gov (NCT03245242)





 720-777-0123
720-777-0123










