- Doctors & Departments
-
Conditions & Advice
- Overview
- Conditions and Symptoms
- Symptom Checker
- Parent Resources
- The Connection Journey
- Calm A Crying Baby
- Sports Articles
- Dosage Tables
- Baby Guide
-
Your Visit
- Overview
- Prepare for Your Visit
- Your Overnight Stay
- Send a Cheer Card
- Family and Patient Resources
- Patient Cost Estimate
- Insurance and Financial Resources
- Online Bill Pay
- Medical Records
- Policies and Procedures
- We Ask Because We Care
Click to find the locations nearest youFind locations by region
See all locations -
Community
- Overview
- Addressing the Youth Mental Health Crisis
- Calendar of Events
- Child Health Advocacy
- Community Health
- Community Partners
- Corporate Relations
- Global Health
- Patient Advocacy
- Patient Stories
- Pediatric Affiliations
- Support Children’s Colorado
- Specialty Outreach Clinics
Your Support Matters
Upcoming Events
Colorado Hospitals Substance Exposed Newborn Quality Improvement Collaborative CHoSEN Conference (Hybrid)
Monday, April 29, 2024The CHoSEN Collaborative is an effort to increase consistency in...
-
Research & Innovation
- Overview
- Pediatric Clinical Trials
- Q: Pediatric Health Advances
- Discoveries and Milestones
- Training and Internships
- Academic Affiliation
- Investigator Resources
- Funding Opportunities
- Center For Innovation
- Support Our Research
- Research Areas

It starts with a Q:
For the latest cutting-edge research, innovative collaborations and remarkable discoveries in child health, read stories from across all our areas of study in Q: Advances and Answers in Pediatric Health.


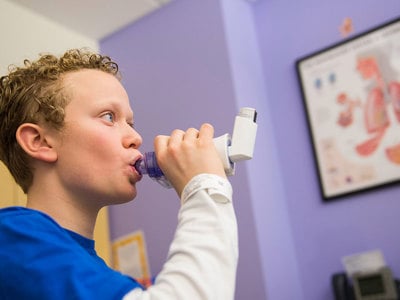
What Parents Need to Know About Asthma in Kids

Asthma is one of the most common chronic conditions in children. According to data from the Centers for Disease Control and Prevention, 6.5% of kids have asthma — that’s more than 4.6 million children across the U.S.
While there’s no cure for the condition, kids with asthma can and do live active, healthy lives. The key is to work with your healthcare provider to create an asthma action plan that guides you and other caregivers on how to manage your child’s asthma. This can include a combination of medications and treatments and other adjustments to avoid asthma triggers.
Below, our pediatric experts share more about asthma in kids — from symptoms and diagnosis to how to effectively manage the condition.
What is asthma, exactly?
In short, asthma is a chronic condition that causes inflammation in the airways, or breathing tubes, in the lungs, says Emily Skeen, MD, pediatric pulmonologist in the Breathing Institute at Children’s Hospital Colorado. When a child has asthma, it can impact the entire airway — from the trachea or windpipe at the top, all the way down to the smaller breathing tubes in the lungs.
Asthma causes breathing difficulties in kids, especially when they are exposed to triggers, such as allergens, exercise, smoke, colds and other viral illnesses. These triggers can make the muscles around the outside of the breathing tubes clamp down, restricting the airways and causing a cough or breathing difficulties.
What are common asthma symptoms in kids?
Shortness of breath, chest tightness, wheezing and difficulty breathing are all common symptoms of asthma in kids; however, Dr. Skeen says that a persistent cough is one of the primary symptoms that is often overlooked, ”particularly, a dry cough that lasts for several weeks and doesn't go away or a cough that is worse at night.” Other symptoms to look out for include coughing, wheezing or difficulty breathing when a child is active and frequent respiratory illnesses or pneumonia.
Many symptoms of asthma overlap with symptoms of respiratory illnesses, such as the common cold, flu, respiratory syncytial virus (RSV) or COVID-19. But Dr. Skeen notes that asthma becomes a concern when a patient has a persistent cough and noticeable wheezing during a lung exam. “Oftentimes, it takes that doctor listening and looking for things for them to be worried about asthma,” she says. That’s why it’s important to see a healthcare provider if your child is experiencing any of the above symptoms on a regular basis or when they’re not sick.
What are some risk factors for asthma in kids?
Doctors are not sure why some kids get asthma. However, there are some factors that increase the chances that a child could develop the condition.
According to the CDC, asthma is more common in male than female children. This reverses in adulthood, where more females are diagnosed with asthma than males. Children who are experiencing poverty are also more likely to have asthma.
There are racial disparities in asthma, as well. Kids who are Black, Hispanic, Native American or Alaskan Natives are more likely to be diagnosed with asthma than kids who are white. Puerto Ricans have the highest rate of asthma of any racial or ethnic group in the U.S. According to research from the Asthma and Allergy Foundation of America, these disparities persist due to several factors — from genetics to home and neighborhood environments to structural racism and healthcare access.
Other risk factors for asthma include:
- Genetics
- A history of allergies or eczema
- Living in an urban environment or near a highway
- Chronic exposure to pollutants
- Being overweight or obese
- Smoking or being exposed to secondhand smoke
At what age are children usually diagnosed with asthma?
“There's a myth that goes around that you can't have asthma if you're too young. Really, you can have asthma at any age,” Dr. Skeen says. “But it is trickier to diagnose in younger kids.” That’s because younger kids are more likely to cycle through respiratory viruses that have symptoms similar to asthma.
Generally, most kids are diagnosed with asthma in lower elementary school or late toddler years, but it is possible to receive an asthma diagnosis at any age.
How is asthma diagnosed in kids?
Even if a child has asthma symptoms, it can be difficult to get an official diagnosis, especially in kids younger than age 6. Dr. Skeen recommends starting with your primary care physician, who will ask you questions about the symptoms, perform a physical exam and take a complete family history. Your doctor might refer you to a pulmonologist or allergist who specializes in asthma, such as those in the Asthma Program at Children’s Colorado.
“An asthma diagnosis can often be made without any special tests,” says Dr. Skeen. “But sometimes we use tests as tools to help us with the diagnosis.” The most common test is pulmonary function testing, or spirometry, which can be performed in kids over age 5. During this test, kids breathe into a tube to measure their lung function. “But that test is not the only way to diagnosis asthma, and sometimes that test is normal, even when the child has asthma,” Dr. Skeen says.
Sometimes, in cases where it’s not clear if a child’s symptoms are associated with asthma, a doctor may prescribe an asthma medication to see how the child responds to it. If they’re doing better while on the medicine, then that helps confirm the diagnosis.
How are asthma and allergies related?
Most people who have asthma also have allergies, but not all people with allergies have asthma. Allergic asthma, when symptoms are worsened by allergens, is the most common kind of asthma in kids.
“When kids have allergic asthma, they'll have certain allergy triggers that make their asthma worse, such as pet dander or pollen,” says Dr. Skeen. If a child with asthma is constantly exposed to irritating allergens, it can cause chronic inflammation in the lungs and worsen symptoms. Or, if they’re suddenly exposed to an allergen — for example, if a child is allergic to cats and they’re not usually around one — it can trigger an attack.
What are common asthma triggers?
Children with asthma have sensitive airways and many things around them can make their condition worse or trigger an attack — a sudden and severe reaction when the airways swell and narrow, making it hard to breathe.
Each child's triggers are different. The best way to reduce asthma symptoms is by knowing and avoiding the things that irritate your child’s airways. Here are some common triggers and how to avoid them.
Allergen triggers
- Household dust and dust mites
- Dust and vacuum often, especially if you have carpets and rugs.
- Make sure your mattresses have allergen-proof coverings.
- Mold or mildew
- Scrub with a sponge and white vinegar to kill mold.
- Fix all water leaks and remove standing water.
- Environmental allergies
- Keep your child's bedroom windows closed during allergy season.
- Have your child shower and change clothes right away after being outside during high-pollen seasons.
- Talk to your child's medical provider about allergy medicines and saline nasal rinses.
- Pets and pet dander
- Keep pets out of your child's bedroom.
- Have your child wash their hands and change clothes after playing with pets.
- Cockroaches
- Keep your house and floor clean and food containers and garbage cans sealed.
- Use insect spray to get rid of cockroaches in your home.
Environmental triggers
- Smoke of all kinds
- Do not allow smoking (tobacco, marijuana or vaping) inside your home or car. If you can, quit smoking. Call 1-800-QUIT-NOW (1-800-784-8669) for help from the QuitLine.
- Do not use a wood-burning stove or fireplace.
- Avoid campfires.
- Stay inside with the doors and windows shut if there is wildfire smoke in your area.
- Air pollution
- Keep an eye on the air quality in your area, and have your child stay indoors when the Air Quality Index is orange or above.
- Strong smells
- Do not use air fresheners, perfume, cologne, room spray or hair spray.
Other asthma triggers
- Illnesses
- Watch your child's asthma closely whenever they have cold and flu symptoms.
- Make sure your child is up to date on vaccinations, including their annual flu shot and COVID-19 boosters.
- Cold air
- When it’s cold outside, ask your child to wear a scarf or neck warmer around their face.
- Have your child breathe through their nose when outdoors in cold air.
- Exercise
- Give your child a quick-reliever medication 10-15 minutes before physical activity to avoid symptoms.
- Strong emotions
- Teach your child calming methods when they feel strong emotions, like getting very angry, scared or sad.
- Practice deep breathing with your child in times when they’re calm and regulated.
What about gas stoves?
You may have heard news recently about a study that showed a link between gas stoves and asthma in kids. While there’s been plenty of research about this topic in recent years, the latest study, published in the International Journal of Environmental Research and Public Health in late 2022, found that 12.7% of childhood asthma cases in the U.S. can be attributed to gas stove use. That’s because gas stoves emit pollutants like nitrogen dioxide and carbon monoxide into the air, which are known to cause respiratory issues in children and adults with breathing problems.
“The connection is concerning,” says Dr. Skeen. “There is a link between the quality of indoor air and kids ultimately going on to develop asthma. So, I think there's certainly a very real risk.”
But Dr. Skeen says you don’t necessarily need to get rid of your gas stove to protect your kids. “Good ventilation in your kitchen is key,” she explains. Make sure you’re turning on the exhaust fan and opening windows every time you use a gas stove.
What is the treatment for asthma?
The treatments for asthma depend on the severity and frequency of a child’s symptoms, as well as the age of the child, Dr. Skeen says. For kids with frequent or severe asthma symptoms and/or attacks that require care in the ER or a hospital stay, doctors usually prescribe a daily asthma medication. This treatment, known as a controller medication, helps calm inflammation in the lungs. They will also likely prescribe a rescue inhaler, known as a bronchodilator, to provide quick relief when symptoms flare up. For kids who have mild or rare asthma symptoms, a doctor might only prescribe a rescue inhaler. If your child is prescribed a rescue inhaler, make sure they have it with them at all times.
There are also combination asthma medications available, which provide a rescue medication and anti-inflammatory medication in a single inhaler. Dr. Skeen says these are sometimes prescribed to older kids as their only medication. For toddlers, asthma medications might only be needed when the child gets sick, especially if that’s their only asthma trigger.
In any case, getting appropriate treatment is crucial. Without it, asthma can lead to decreased lung function over time and affect a child's ability to participate in sports and other activities.
What is an asthma action plan?
An asthma action plan is a document created with your child’s doctor to help guide you and other caregivers in effectively managing your child’s asthma. Asthma action plans use a stoplight format for easy understanding.
- Green zone: When your child is in the green zone, they're healthy and doing well. The plan outlines the things you or your child need to do to help them stay well, such as taking medications or avoiding triggers.
- Yellow zone: When a child is in the yellow zone, you might notice some asthma symptoms, such as increased coughing, wheezing or shortness of breath, but they're not experiencing an emergency. In this zone, your doctor might recommend using a rescue inhaler more frequently or starting an additional medication.
- Red zone: This is when an asthma attack becomes an emergency. In this zone, your healthcare provider will suggest things you can do at home and provide guidance on when to call 911 or seek emergency care.
Make sure your child’s asthma action plan is easily accessible, and that you have a copy on file with the nurse at your child’s school.
Can you grow out of asthma?
Some children do “outgrow” asthma. Others, especially those with allergies or whose parents have asthma, are less likely to outgrow it. However, symptoms can improve over time.
“If you have persistent asthma at the age of 6, generally, we think of asthma as being lifelong,” Dr. Skeen says. “That said, the severity of asthma varies dramatically. A lot of people's asthma gets a lot better as they get older.” This might be because they're experiencing fewer triggers as they move into adulthood, such as viruses and increased activity. For those who have fewer symptoms as they get older, they might still need quick-relief medicine like albuterol when they are sick with a cold or to get relief from certain triggers.



 720-777-0123
720-777-0123