- Doctors & Departments
-
Conditions & Advice
- Overview
- Conditions and Symptoms
- Symptom Checker
- Parent Resources
- The Connection Journey
- Calm A Crying Baby
- Sports Articles
- Dosage Tables
- Baby Guide
-
Your Visit
- Overview
- Prepare for Your Visit
- Your Overnight Stay
- Send a Cheer Card
- Family and Patient Resources
- Patient Cost Estimate
- Insurance and Financial Resources
- Online Bill Pay
- Medical Records
- Policies and Procedures
- We Ask Because We Care
Click to find the locations nearest youFind locations by region
See all locations -
Community
- Overview
- Addressing the Youth Mental Health Crisis
- Calendar of Events
- Child Health Advocacy
- Community Health
- Community Partners
- Corporate Relations
- Global Health
- Patient Advocacy
- Patient Stories
- Pediatric Affiliations
- Support Children’s Colorado
- Specialty Outreach Clinics
Your Support Matters
Upcoming Events
Public Meeting: 2024 Community Benefit and Hospital Transformation Program
Tuesday, May 14, 2024Join Children's Hospital Colorado at one of our virtual events to learn...
-
Research & Innovation
- Overview
- Pediatric Clinical Trials
- Q: Pediatric Health Advances
- Discoveries and Milestones
- Training and Internships
- Academic Affiliation
- Investigator Resources
- Funding Opportunities
- Center For Innovation
- Support Our Research
- Research Areas

It starts with a Q:
For the latest cutting-edge research, innovative collaborations and remarkable discoveries in child health, read stories from across all our areas of study in Q: Advances and Answers in Pediatric Health.


Joey and Paul: Surviving Twin-to-Twin Transfusion Syndrome

The wishes and prayers of my husband Robert and I have always been to fill a house with little feet. Our first blessing was the birth of twin boys, who alone certainly guaranteed a busy house. But the following year, in March of 2013, I became pregnant again. We were beyond thrilled – and happily surprised – to learn that, by the end of the year, we would welcome a second set of twin boys.
My first pregnancy had been rough – I was sick pretty much the entire time. On multiple occasions, I was hospitalized for severe dehydration and was even put on bed rest at 26 weeks. Now a year later, with a second twin pregnancy, I was in a similar position. But I could tell something was not right this time. I felt changes in my body different than that of a normal pregnancy. The swelling was significant. My mobility was severely compromised and I generally felt worse than with my previous pregnancy.
And so shortly afterward, a 25-week routine ultrasound revealed a frightening diagnosis: Our boys had a disproportionate amount of fluid between the two of them. It was, as we were told, textbook twin-to-twin transfusion syndrome, a condition that affects twins sharing a placenta. The shared placenta contains abnormal blood vessels, which affects the fluid balance between the two. Our one twin, Joey, had more blood vessels than his brother Paul. Joey’s tiny body had to work twice as hard to process all the fluid and nutrients flowing through his blood vessels, whereas our other twin, Paul, had to survive with much less.
Within an hour of the diagnosis, the team at the Colorado Institute for Maternal and Fetal Health (a partnership between Children’s Hospital Colorado and the University of Colorado Hospital) had a plan for saving our boys’ lives. We understood that there wasn’t much time to lose. On the way home from the meeting, I received a call from the case manager who explained I should arrive at the hospital the next day to meet with the entire team: fetal surgeons, pediatric cardiologist, ultrasound technicians, nurses, facilitators and case workers. A series of appointments had already been scheduled and I would be in the operating room within 36 hours of diagnosis. At a time of uncertainty, our fear was quickly replaced with trust and confidence.
Meeting with Dr. Michael Zaretsky (a maternal fetal medicine physician) and Dr. Timothy Crombleholme gave our family a sense of peace. I remember clearly Dr. Crombleholme looking at us as he discussed our situation. “I know what this is,” he said with his quiet confidence and soft-spoken voice, “and I know how to fix it.”
Surgery to treat twin-to-twin transfusion syndrome
To highly emotional expectant parents, there was nothing better than to hear Dr. Crombleholme’s words. At the same time, we were facing a dangerous and deadly fetal condition. Twin-to-twin transfusion syndrome (or TTTS) can cause the death of one or both twins – only a few decades ago, the fetal anomaly was almost always likely to claim both lives.
The fetal intervention was scheduled, and I was prepared for the procedure. A highly educated, extremely talented team of men and women performed a laser procedure which would even out the fluids between our boys. Paul would have the nutrients he needed to survive, while easing the strain on his brother’s tiny organs.
By that afternoon I felt so much better. The swelling began to subside. The dehydration was gone. My mobility returned. We were on our way. Five days later I came home to my two older boys and happily waited for the arrival of Joey and Paul. But two weeks later, just 27 weeks pregnant, my water broke. Surprisingly, this does not mean immediate labor. I was once again admitted to the anti-partum floor of the hospital where I remained until I delivered at 29 weeks and one day. On September 13, 2013, amidst an epic Colorado rainstorm, Joey and Paul entered the world. Weighing just over three pounds each, my boys were premature, but alive. Our prayers had been answered.
Life after TTTS
The day before Halloween, after a six-week stay in the NICU, our boys came home. Their brothers, only 20 months old at the time, were completely fascinated with their new roommates. At long last, we were all under one roof together.
Today, a chorus of many little feet is often heard around our house. Joey and Paul have rebounded to normal weights – and normal lives. They are incredibly happy boys who love balls, bananas, books, Mickey Mouse and most of all, their older twin brothers. They show no sign of prematurity, neither in size nor development. They laugh, eat heartily, sleep soundly and bring us tremendous joy each day.
As for our gratitude, “thank you” has never seemed so inadequate. Because of the team at the Colorado Institute for Maternal and Fetal Health, my boys will live happy lives. They will play soccer and go skiing. They will swim with their cousins and travel with their grandparents. They will attend kindergarten and go to college, celebrate birthdays, enjoy Christmas and play in the snow. Because as one of the fetal surgeons explained, the team doesn’t just save lives, they save lifetimes.
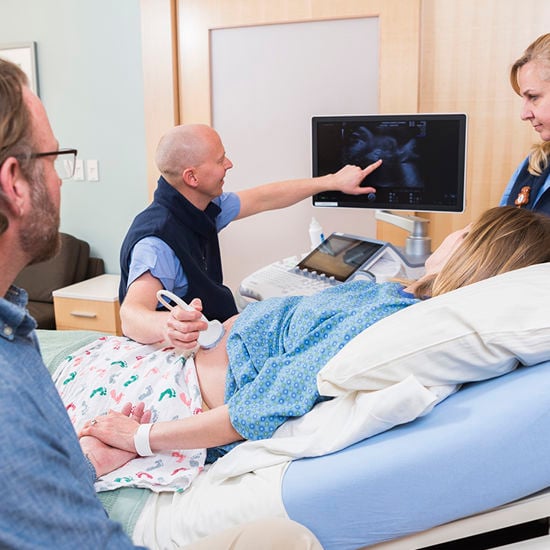
Would you like a second opinion?
If you have received a prenatal diagnosis, are considering treatment options or just want to feel more confident about your treatment plan, our fetal care experts are here to help.
Request a second opinion from our Colorado Fetal Care Center



 720-777-0123
720-777-0123



